[Feature] A New Paradigm in Emergency Diagnosis: Kyung Hee Researchers Develop the World’s First Bioadaptive Multimodal Sensor
A collaborative research team led by Jin Sung-hun, a professor in the Dept. of Future Information Display at Kyung Hee University, along with Dr. Seo Seung-gi from Prof. John A. Rogers' team at Northwestern University, Kim Seung-yeop, a researcher from KAIST, Prof. Yoo Seong-gwang from Inje University, and Prof. Oh Se-yong from Hanyang University ERICA Campus developed the world's first ultra-miniature multimodal sensor technology for the early diagnosis of Acute Compartment Syndrome (ACS).
The research was supported by the National Research Foundation of Korea, funded by the Ministry of Science, ICT and Future Planning. It was published in Advanced Science on July 17, 2025, under the title, Minimally Invasive, Bioadaptive Multimodal Sensor Probe with Safe Deployment for Real-Time Acute Compartment Syndrome Diagnosis.

Photo: Advanced Science (advanced.onlinelibrary.wiley.com)
Measuring Pressure, Blood Flow, and Oxygen Saturation—All at Once
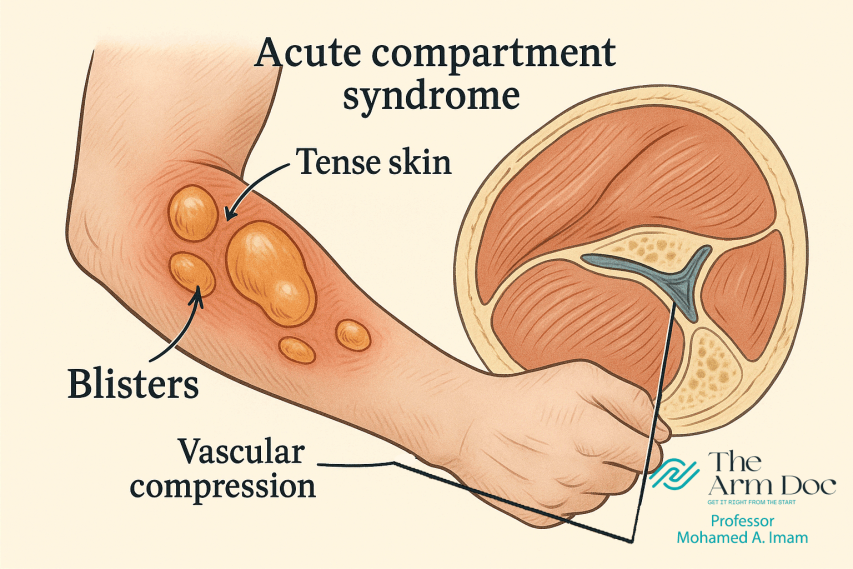
Acute Compartment Syndrome (ACS) is a critical condition in which pressure builds up inside a closed muscle compartment, cutting off blood flow and damaging surrounding tissues. Without timely diagnosis, it can cause irreversible nerve and muscle damage or even lead to limb amputation. Despite its severity, ACS is still diagnosed mainly through qualitative assessments such as a patient’s pain or sensory changes, along with occasional pressure measurements. These methods are often unreliable and may fail to identify ACS within the critical window for intervention.
Symptoms like pain, paresthesia, and paralysis tend to appear only in advanced stages, while vascular signs—such as pallor or absent pulse—often emerge too late for successful intervention. As a result, physicians frequently face uncertainty in determining whether surgery is necessary. This can lead to two equally serious outcomes: missed diagnoses that result in limb loss, or unnecessary and disfiguring surgeries performed when ACS is not actually present.
Acute Compartment Syndrome
Photo: The Arm Doc (thearmdoc.co.uk)
Prof. Jin noted that this diagnostic dilemma served as the starting point for the research. “The question of how to make accurate and timely decisions for ACS was precisely the background for this study,” he said. To address these challenges, the research team designed an innovative multimodal sensor capable of simultaneously measuring compartment pressure, tissue oxygen saturation (StO₂), and blood flow—paving the way for a more objective and real-time diagnostic standard.
Ensuring Safe Insertion and Stable Measurement with PASI Design
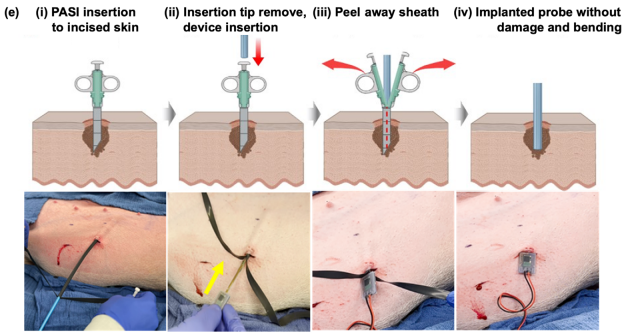
Step-by-step procedure for minimally invasive deployment of the multimodal sen sor probe
Photo: Advanced Science (advanced.onlinelibrary.wiley.com)
To address the diagnostic limitations described above, the research team developed an ultra-miniature multimodal sensor probe that measures not only compartment pressure but also StO₂ and blood flow at the same site in real time. This approach allows physicians to assess multiple physiological indicators simultaneously, providing a more comprehensive and accurate diagnosis. The newly developed probe is remarkably compact—only 4 millimeters in diameter and 1 millimeter thick—and is made from flexible, biocompatible materials that can safely be inserted into the human body. With just a single insertion, the device captures three different types of biological information and transmits them wirelessly in real time via Bluetooth Low Energy. This real-time data collection enables faster clinical decisions and reduces the likelihood of missed or delayed diagnoses.
Beyond developing the sensor itself, the team focused heavily on how to safely insert and remove the device once measurements are complete. To address this, they introduced a Peel-away Sheath Introducer (PASI) system, which is originally used in medical catheter procedures. “Building the sensor is important, but what truly matters is how it can be inserted and removed safely after evaluation,” Prof. Jin explained. It allows the sensor to be placed stably during insertion and removed just as smoothly afterward, he compared to peeling a banana. This peel-away mechanism ensures that the sensor can penetrate dense tissue without damage and remain stable during measurement. He emphasized that while the PASI concept already existed in the medical field, his team was the first to apply it to a multimodal sensor platform, enhancing both safety and practicality.
Photo: Advanced Science (advanced.onlinelibrary.wiley.com)
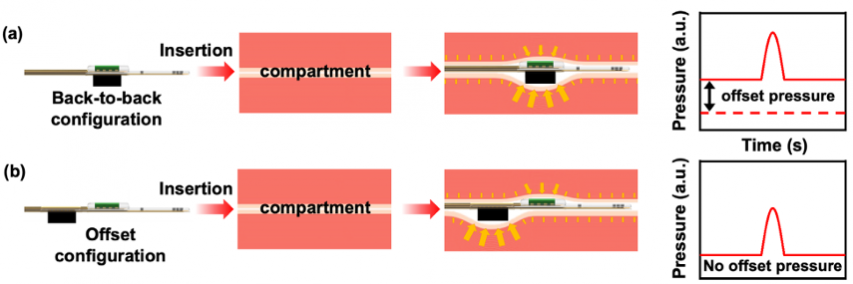
Another key challenge was minimizing interference between sensors when measuring three physiological signals simultaneously. In the early stages, the team experimented with a back-to-back configuration—placing the pressure and oxygen sensors facing each other—but found that mechanical interaction caused offset pressure and inaccurate readings. “When the sensors were aligned facing each other, pressing one would create rebound force that compromised the accuracy of the other’s measurements,” Prof. Jin explained. “To fix this, we reconfigured the sensor layout using an offset design, which significantly improved measurement accuracy," he added.
By redesigning the sensor structure, the team minimized signal interference and achieved stable readings for multiple physiological indicators in real time. Prof. Jin added that while inserting the device may require a small incision, it can remain inside the body for continuous monitoring. “Our device allows continuous monitoring inside the body, helping doctors decide early whether surgery is truly necessary. This approach can reduce both diagnostic delays and unnecessary fasciotomies, easing the patient’s burden overall,” he emphasized.
One Study, Three Directions: Medical, Engineering, and Educational Impact
The research team validated the sensor’s stability and performance through in vivo tests using animal models. Even under simulated compartment syndrome conditions, the device successfully transmitted accurate physiological data in real time, confirming its reliability and biocompatibility. From an academic standpoint, Prof. Jin highlighted that the study’s significance lies in establishing a multiphysics framework that integrates mechanical, thermal, electrical, and material perspectives into one miniature platform. “This research required more than simply combining sensors,” he explained. “We had to understand and model how mechanical forces, heat, and electrical signals interact within an extremely small space." He added that the process deepened their understanding of multiphysics behavior and demonstrated how stability, safety, and wireless operation can coexist in one bioadaptive system.
From a practical perspective, the study also opens possibilities far beyond clinical diagnosis. The sensor’s multimodal measurement principle—simultaneously tracking pressure, temperature, and flow—can be adapted for a wide range of applications, from structural health monitoring in heritage architecture to pipeline safety and environmental sensing. “This technology is not limited to the human body,” said Prof. Jin. “Imagine embedding similar sensors in wooden structures like ancient temples to monitor internal pressure or temperature changes over time, or in oil pipelines to detect leaks and flow variations. The same core principle can be applied in countless fields.”
Beyond engineering, Prof. Jin envisions this platform as an educational tool that nurtures interdisciplinary thinking among younger generations. His lab is exploring ways to integrate eco-friendly and hands-on scientific modules into Science, Technology, Engineering, and Mathematics (STEM) education, helping students connect materials science, electronics, and bioengineering through hands-on, interactive kits. “Our goal is not just to develop technology, but to cultivate curiosity,” he said. “By turning these platforms into learning tools, we can inspire students to think across disciplines—from physics and chemistry to data science—and help them build creative confidence in solving real-world problems.”
The study proposes a new diagnostic standard in emergency medicine, overcoming the limitations of existing invasive diagnostic methods. This technology fundamentally addresses the constraints of conventional approaches reliant on fragmented data by simultaneously quantifying multiple vital signs through a single probe. Its significance lies in presenting a next-generation clinical tool that enables early and accurate ACS diagnosis, reducing unnecessary surgeries and improving patient outcomes. Such advances could greatly contribute to lowering misdiagnosis rates and facilitating early treatment decisions in emergency settings.
The study represents more than a technological advance. It introduces a new paradigm for bioadaptive sensor systems that merge diagnostic precision, interdisciplinary research, and educational value. Prof. Jin concluded by encouraging students to step beyond familiar surroundings—to build their abilities, learn from good mentors, and seek broader experiences both in Korea and abroad.
There are no registered comments.
I agree to the collection of personal information. [view]