[Feature] Suggesting the Future Direction of Gut Microbiome Therapy: Insights from Bae Jin-Woo’s Study
Professor Bae Jin-Woo from the Dept. of Biology and his research team have published a study examining the efficacy and limitations of two microbiome therapies: Fecal Microbiota Transplantation (FMT) and Live Biotherapeutic Products (LBPs). Their findings, titled Gut Microbiome Therapy: Fecal Microbiota Transplantation vs. Live Biotherapeutic Products, were published in Gut Microbes on October 8, 2024. Unlike previous studies that focused solely on each treatment, this research provides a comparative analysis of the two approaches.
Photo: Microba Life Sciences (insight.microba.com)
FMT and LBPs, Widly-use Treatment to Balance Gut Microbes
Gut microbes play a crucial role in the human body. The term gut microbes refer to microorganisms that live in the digestive organs of humans and animals. The imbalance can lead to various issues, including aging, diabetes, obesity, cancer, stress-related diseases, and inflammatory bowel disease.
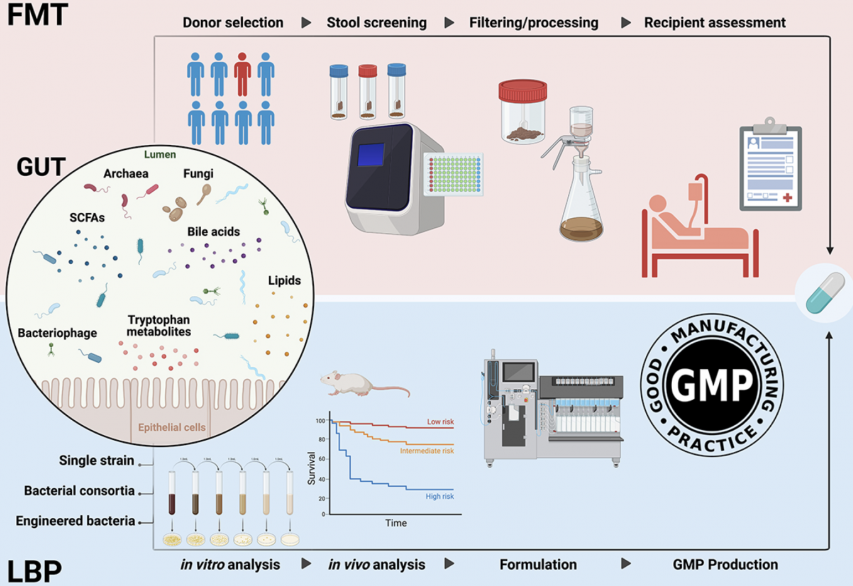
As the intestinal environment is linked to health, some treatments have been used to adjust the bacteria living in the gut. Among them, FMT and LBPs are the most well-known. FMT is a method that transplants entire gut microbes from a healthy person. It has been approved as a medical product by the U.S. Food and Drug Administration (FDA) since 2013. In contrast, LBPs are biological products containing living microbes and have also been approved for medical use.
However, despite these approvals, the process of administering FMT and LBPs remains underdeveloped. Due to its complexity, FMT lacks clear guidelines on manufacturing and usage. While LBPs are approved as medical products, many commercial companies bypass rigorous safety and efficacy evaluations, instead marketing them as simple dietary supplements. These gaps highlight the need for further studies to assess the safety and effectiveness of both treatments.
Photo: Kyung Hee University (khu.ac.kr)
Findings of the Microbiome
The study examined the potential of FMT and LBPs as treatments for digestive system diseases, particularly Clostridioides difficile infection (CDI) and inflammatory bowel disease (IBD). CDI is a bacterial infection that affects the colon and can cause symptoms ranging from mild diarrhea to serious health complications, such as kidney failure. The study found that FMT is a more effective treatment than antibiotics, which are commonly used to treat the disease. It also suggested that LBPs might work in a similar way. Researchers explained that the mechanism of these treatments involves generating beneficial substances, such as short-chain fatty acids, and helping maintain bile acid balance, which determines whether infection spreads or worsens.
IBD is a disease that affects the digestive system and includes two main types: ulcerative colitis (UC) and Crohn’s disease (CD). Both conditions share common features, such as long-term inflammation, flare-ups, and a significant impact on daily life. The study found that FMT had a high success rate in reducing symptoms like stomach pain and diarrhea. Additionally, it showed that several medicines used for LBPs have been effective in past studies, but they have not yet been officially approved for use.
The microbiome is linked not only to intestinal diseases but also to metabolic diseases. The study found that gut bacteria can influence conditions such as obesity, metabolic syndrome, type 2 diabetes (T2D), and certain liver diseases. Past research showed that FMT can impact factors related to metabolic diseases, such as weight gain or loss, blood sugar levels, insulin resistance, and inflammation. Additionally, certain LBPs have been found to regulate bad cholesterol, fibrinogen levels, lipid levels, and fat-related inflammation, contributing to the treatment and improving T2D and liver diseases. However, some studies did not find FMT or LBPs effective in improving obesity and metabolic syndrome, highlighting the need for further research.
The human body has a gut-brain axis, a two-way communication system connecting the gut and brain. This connection means gut bacteria may also play a role in neurological diseases like autism spectrum disorder (ASD), Alzheimer’s disease (AD), and Parkinson’s disease (PD).
The study found that FMT is effective for ASD, improving both digestive and behavioral symptoms. For AD, FMT has shown positive effects by reducing harmful brain plaques and enhancing memory. Some studies also suggest that LBPs could help treat AD, but no officially approved treatment exists yet.
For PD, FMT has only been proven to relieve gut-related issues like constipation, a common symptom of the disease. The team emphasized the need for further studies to determine whether it can directly help treat PD.
Furthermore, Cancer, a life-threatening disease, is also relevant to gut bacteria. The research found that FMT and LBPs could improve the effectiveness of cancer treatments like chemotherapy, immunotherapy, and radiation therapy. Additionally, these bacteria may help reduce side effects, such as inflammation that can occur during cancer treatment. These findings have been proven in early studies on both animals and humans, but the effectiveness varies from person to person.
Problems with Gut Microbiome Therapy
Despite these findings, the team pointed out several shortcomings that need to be addressed in the future. First, a more accurate test for administering FMT is necessary. Since FMT requires stool from a healthy donor, using an unsuitable donor could worsen the disease. This highlights the need for more advanced methods that better support doctors in identifying the right donor.
Additionally, the team suggested that differences in effectiveness based on the method of FMT administration should be studied. Doctors face various questions before using FMT, such as whether to administer fecal matter orally or rectally and whether to use a frozen or fresh sample. Determining the effectiveness of various methods is another important step for the field.
Regarding effectiveness, the team also noted that finding a way to maintain transferred bacteria more stably in the patient’s body is another important consideration.
Lastly, the team pointed out that whether using antibiotics leads to greater effectiveness or contributes to antibiotic-resistant bacteria has not been studied yet.
The Future Direction of These Treatments
As the study is structured as a review paper, Prof. Bae explains its meaning: “Review papers enable comparison, analysis of the longitudinal and cross-sectional facts found in previous studies.” He added, “For example, a substance could work in some research while failing in others, requiring further studies to compare observation environments, subject differences, and other factors that may affect the results.”
Following this approach, the study examines FMT and LBPs, aiming to organize separate findings on these treatments. This comparison seems to help establish a clearer path for future advancements in the field.
Using FMT and LBPs can help treat many diseases by adjusting to the gut environment. While these treatments have shown effectiveness in past studies, challenges remain, requiring more clinical trials with long-term follow-ups to evaluate their benefits and address potential risks. As experts in this field, including Bae’s research team, continue to conduct studies, these treatments appear to be increasingly beneficial in daily life.
There are no registered comments.
- 1
- 2
I agree to the collection of personal information. [view]